Introduction to AMS audit and quality improvement
A quality improvement (QI) audit collects data on a small number of subjects, focusing on key measures of quality of prescribing. QI audits are usually designed to be simple so that they are easy to repeat periodically. This will enable services to document improvement in practices over time and feed into the plan–do–study–act model of QI. Data for improvement measured regularly can be visually displayed with use of run-charts.
| Model for Improvement |
PDSA Cycle |
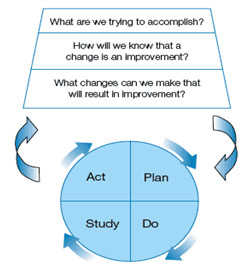 |
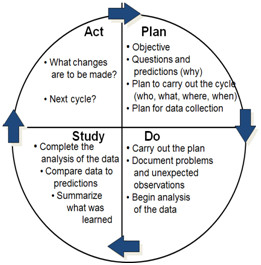
|
Auditing the quality of prescribing can provide assurances that the most effective therapy is being given and that the risk of poor outcomes (including antimicrobial-related adverse events) is being reduced.
Clinical audit allows problem areas to be targeted and enables more intensive examination, leading to further interventions to improve prescribing.
Audit Tools
Preferred antibiotic audit tool
The Preferred antibiotics audit tool involves a self-audit of 10 antimicrobial prescriptions, and encourages general practitioners to reflect on their prescribing behaviour relative to current best-practice guidelines.
An example of a quality improvement project that used this audit tool model is the Out of Hours Antibiotic Stewardship Improvement Project.
Antibiotic UTI prophylaxis audit tool
The aim of this UTI prophylaxis audit tool is to enable review of patients currently prescribed antimicrobials for prophylaxis of urinary tract infections (UTIs). Further instructions and guidance can be found within the tool. You can download and use the antibiotic UTI prophylaxis audit tool here:
Azithromycin prophylaxis in adults with respiratory disease audit tool
The azithromycin prophylaxis audit tool is available to support healthcare professionals reviewing patients on azithromycin prophylaxis. For more information, visit the azithromycin prophylaxis in adults with respiratory disease guideline page.
Surgical antibiotic prophylaxis audit tool
An excel audit tool and a YouTube video explaining its use are available to support the implementation of the joint position statement on surgical antibiotic prophylaxis as part of a quality improvement project. For more information visit the Surgical Antibiotic Prophylaxis page.