Benefits
The National Clinical Programme for Epilepsy is to deliver these objectives by addressing each aspect of care with a specified care pathway and delivered by experts in epilepsy care, leading to benefits for patients and carers
Establishment of network of Epilepsy Centres
Epilepsy Centres staffed by a new cohort of epilepsy experts from a nursing background (RANPs) who will be the main contact within the group for expert services. Working in tandem with medical consultants and epilepsy Non-Consultant Hospital Doctors (NCHD’s), they will provide routine epilepsy care in the epilepsy centres including in and outpatient care, begin providing rapid access service for community and emergency department (ED) referrals, telephone, email and web-based advice. In time they will provide outreach services to secondary care hospitals, maternity hospitals, intellectual disability services and primary care centres.
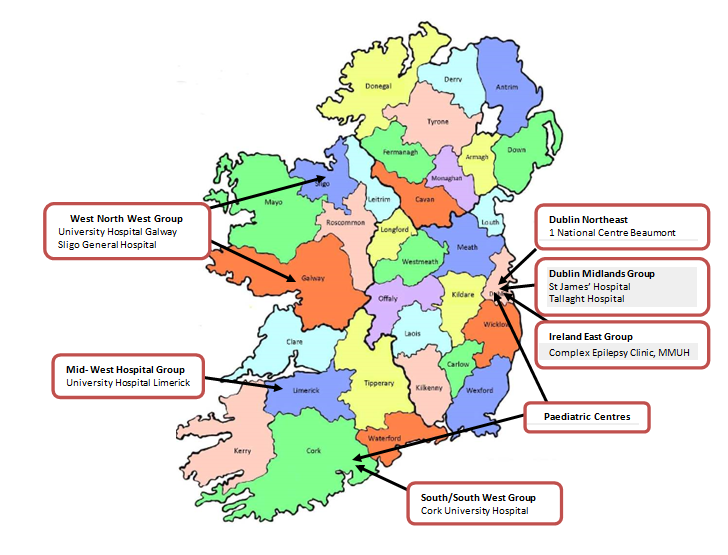
Population-based nurse-led service
Every patient with epilepsy in Ireland will have access to the epilepsy RANP service attached to one of the adult or paediatric centres. Patients attending services outside of their locality will be encouraged to transfer care back to the centre in their local area so as to avail of the RANP service. The nurse-led service will be a protocol-driven, chronic disease model of care covering the following responsibilities:
- Rapid access clinics in acute hospitals providing acute neurological care.
- Outreach clinics. – Intellectual disability services and non-acute hospitals.
- GP and community practice nurse support.
- Liaison with physicians in hospitals without neurology services, and with paediatricians.
- Telephone/e-mail/web support for patients.
- Links to Epilepsy Ireland and the Irish Branch of the International League Against Epilepsy (ILAE).
- Ensure complete, accurate and up-to-date documentation of clinical encounters using an Electronic Patient Record (EPR).
- Implementation of Standard Operating Procedures (SOPs) and management operating procedures (MOPs).
- Use of Electronic Patient Record and Standard Operating Procedures (SOPs) and Management Operating Procedures (MOPs).
- Registration and measurement of Key Performance Indicators, quality outcomes and clinical audit.
- Health Services Research, population health and clinical and translational research.
Structured primary care programme led by GPs in association with the PCT and the RANP epilepsy.
The epilepsy programme takes account of the significant reconfiguration of resources occurring across all hospital sectors to bring services to the community with appropriate care delivered in the community unless acute intervention is required. The programme envisages GPs and other community health workers in each community healthcare organisation having a key role in the delivery of epilepsy care within the community
Seizure Care Pathway for acute hospital based seizure management in ED/AMAU and wards.
Through the use of an integrated care pathway, administered through Emergency Departments (ED) and the AMAUs (Acute Medical Admissions Units), front-line physicians will use an intelligent, evidence-based algorithm to help with management and disposition of patients who come to hospital with first seizures or breakthrough events
Expanded, appropriately resourced, pre-surgical evaluation programme in two centres.
Patients with complex epilepsy requiring pre-surgical workup and evaluation for possible device implantation will be referred to Beaumont and Cork University Hospital (CUH). There will be a 4-bedded video telemetry unit in Beaumont Hospital, and a 2-bedded video telemetry unit in CUH fully staffed with staff nurses.
Delivery of care in the most appropriate setting through access to clinical information when and where needed via an electronic patient record (EPR) (e.g. for community outreach, primary care and hospital-based).
Standardized clinical documentation, sharing and exchange of patient information between clinicians as well as performance monitoring and evaluation are all key to the success of the new model of epilepsy care. This will be facilitated by a secure web-based electronic patient record (EPR) which will provide authorized clinicians, regardless of geographical location, with access to complete and accurate patient records when and where needed.
Countrywide telephone direction for health professional
The Epilepsy programme aims to promote the management of epilepsy at the primary care level by improving the communication between primary and specialist services, and the development of access to guiding information.
Learn more about Transitioning from paediatric to adult service
