Comments from Expert Advisory Group
Nail samples should be taken and treatment started if infection confirmed.
- Most viable fungi are usually found in the most proximal part of diseased nail
- Include full thickness clippings of the diseased nail and subungual debris
- Sample as far back from nail tip as possible, as this is where fungi are usually found; also sample debris from under the diseased part of the nail
- In superficial infections, scrape surface of diseased nail plate with scalpel blade
Concomitant tinea pedis is common and is a risk factor for treatment failure. Tinea pedis should be treated appropriately.
For children seek specialist opinion.
|
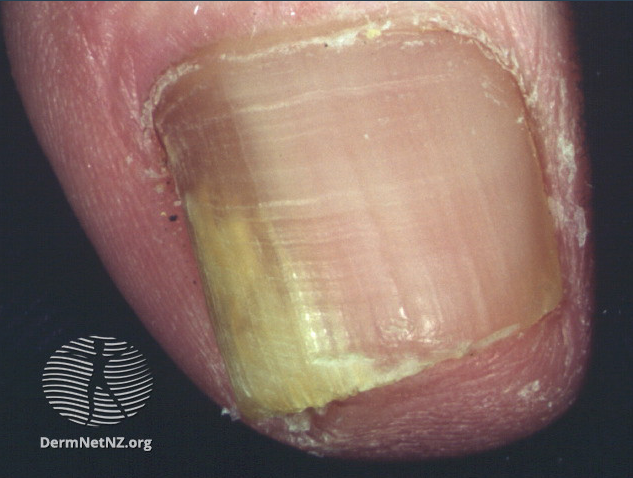
Image 1: Onychomycosis
Images source/credit: Dermnet
|
 |
|
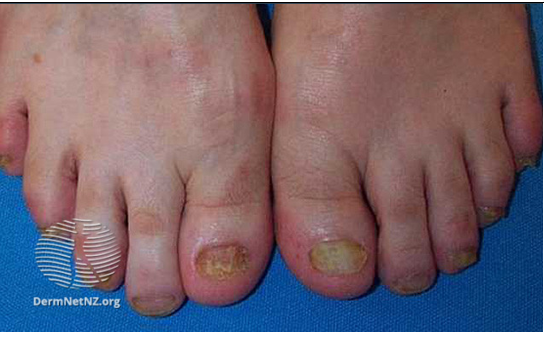
Image 2: Onychomycosis
Images source/credit: Dermnet
|
 |
Treatment
Topical treatments are limited to those specifically licensed for treatment of nail disease, other topical antifungals (e.g. creams) are not suitable as they do not penetrate the nail.
Oral antifungal therapy is considered the gold standard for treatment of onychomycosis, however in cases where there are contraindications for systemic treatment, potential for drug-drug interactions or patient preference, then topical treatment may be considered.
Topical treatment should only be used when less than 50% of the nail is affected and the infection has not spread to the nail matrix and/or lunula.
|
Onychomycosis - Dermatophyte Infection of the Fingernails and Toenails
|
|
Topical treatment
|
|
Drug
|
Dose
|
Duration
|
Notes
|
|
5% amorolfine nail lacquer
|
Apply once weekly
|
Fingernails: 6 months
Toenails: 9–12 months (review at 3 monthly intervals)
|
File down nail surface as much as possible.
Clean and degrease surface of nail with an alcohol cleaning pad.
Apply nail lacquer to entire surface of affected nail(s) using supplied spatula.
Allow to dry for 3-5 minutes.
Filing and cleansing of the nail should occur before each application.
Do not apply nail varnish over the lacquer.
|
|
Oral treatment : 1st choice
|
|
Terbinafine
|
250mg every 24 hours
|
6 weeks to 3 months depending on severity of infection and nail growth
|
Not recommended in patients with active or chronic liver disease.
Pre-treatment LFTs should be performed. If prolonged treatment is required, repeat LFTs after 4-6 weeks is recommended.
Some toenail infections may take more than 6 months to clear.
|
|
Oral treatment : 2nd choice
|
|
Itraconazole* – continuous therapy
|
200mg every 24 hours
|
Fingernail – 6 weeks
Toenail – 12 weeks
|
Take capsules immediately after a meal for maximum absorption.
Not recommended in patients with active or chronic liver disease.
If treatment is for longer than one month then pre-treatment LFTs should be performed and then monitored.
Avoid itraconazole (and all oral azoles) in pregnancy*
|
|
OR
Itraconazole* – pulse therapy
|
Fingernail: 200 mg every 12 hours for one week per month
Toenail: 200 mg every 12 hours for one week per month |
Fingernail: 2 months
Toenail: 3 months
|
| * Women of childbearing potential taking itraconazole should use contraceptive precautions. Effective contraception should be continued until the menstrual period following the end of itraconazole therapy. |
Patient Information
- Doses are oral and for adults unless otherwise stated
- Renal impairment dosing table
- Safety in Pregnancy and Lactation
- Drug interactions table. Extensive drug interactions for clarithromycin, fluoroquinolones, azole antifungals and rifampicin. Many antibiotics increase the risk of bleeding with anticoagulants.
- Visit the Health Products Regulatory Authority (HPRA) website for detailed drug information (summary of product characteristics and patient information leaflets). Dosing details, contraindications and drug interactions can also be found in the Irish Medicines Formulary (IMF) or other reference sources such as British National Formulary (BNF) / BNF for children (BNFC).
Reviewed December 2022
