(tinea corporis, tinea cruris, tinea pedis, tinea manum)
Comments from Expert Advisory Group
Definitions:
Tinea corporis - Infection of body surfaces (other than the feet, groin, face, scalp hair, or beard hair)
Tinea cruris - Infection of the groin
Tinea pedis - Infection of the foot
Tinea manum - Infection of the hand (usually unilateral; if bilateral, usually asymmetrical)
NB: Tinea incognito — inappropriate use of topical corticosteroids can lead to extensive spread of fungal infection, and a change in the morphology of lesions.
For guidance on when to perform skin scrapings, see section below treatment table.
Risk factors include:
- Hot / humid environments
- Wearing tight-fitting clothing
- Obesity
- Hyperhidrosis
Immunocompromised states may lead to severe, resistant or extensive disease.
Children with tinea pedis: consider referral to secondary care.
Self-care management strategies:
- Wear loose-fitting clothes
- Maintain good hygiene by washing affected skin areas daily
- After washing dry thoroughly, especially in the skin folds
- Avoid scratching affected skin, as this may spread infection to other sites
- Do not share towels, and wash them frequently, to reduce the risk of transmission
- For tinea pedis put on socks prior to underwear to reduce risk of fungal carriage to the groin
Wash clothes and bed linen frequently to eradicate fungal spores.
|
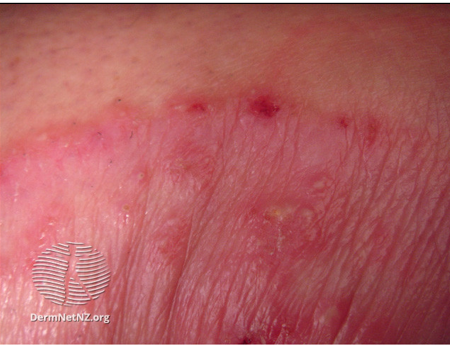
Image 1 Tinea corporis: Sharp red scaly margin of tinea corporis
Image source: Dermnet
|
 |
|
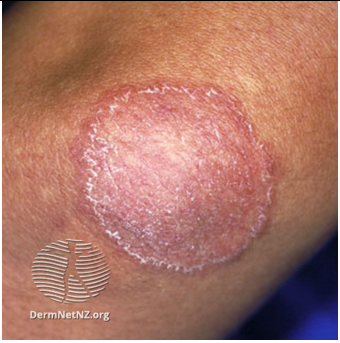
Image 2: Tinea corporis
Image source: Dermnet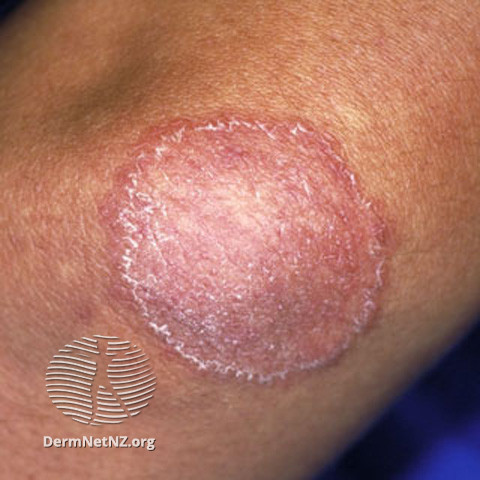
|
 |
|
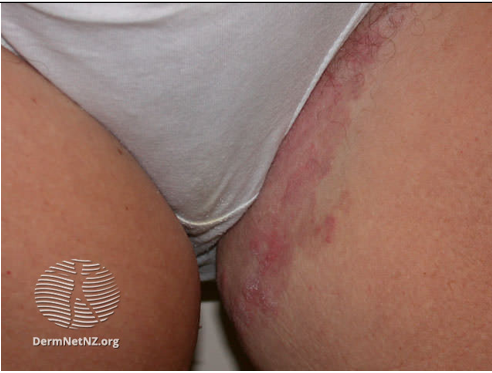
Image 3: Tinea cruris: Unilateral rash in the groin
Image source: Dermnet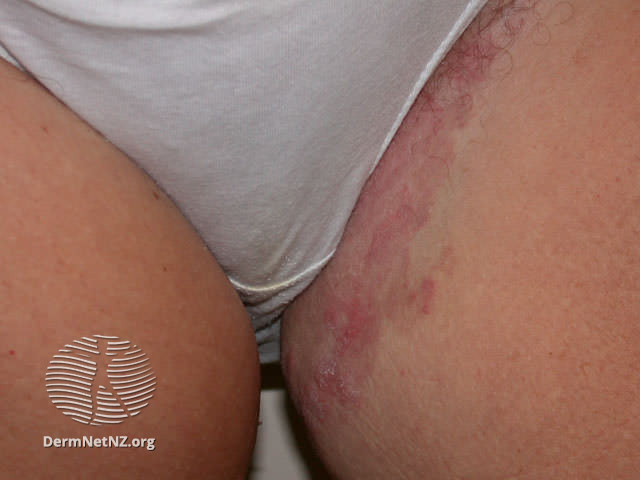 
|
 |
|
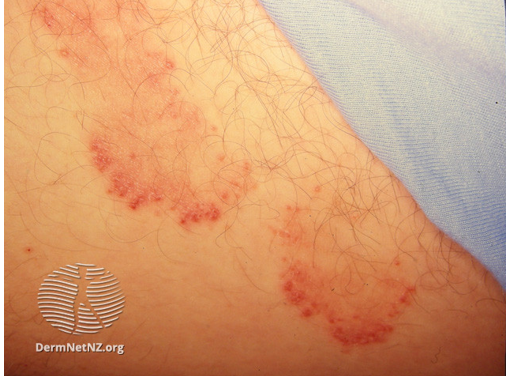
Image 4: Tinea cruris: Raised border and central clearing
Image source: Dermnet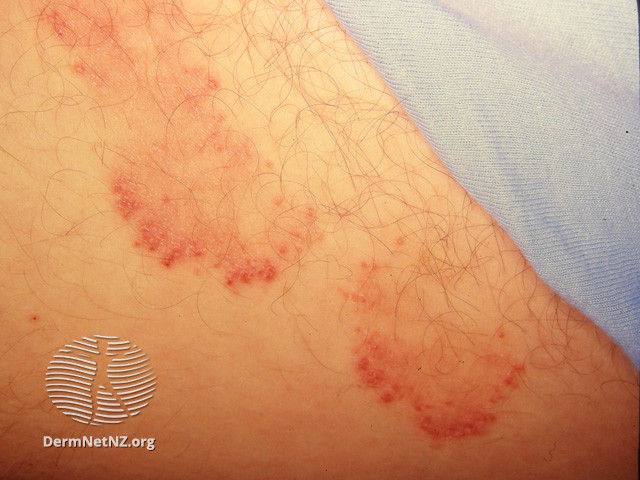 

|
 |
|
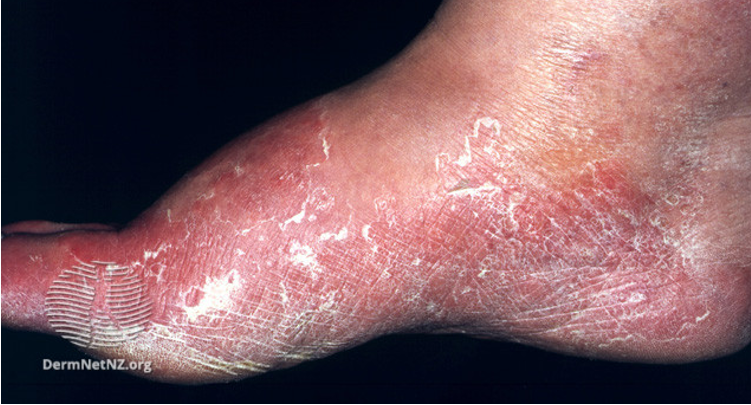
Image 5: Tinea pedis
Image source: Dermnet
|
 |
|
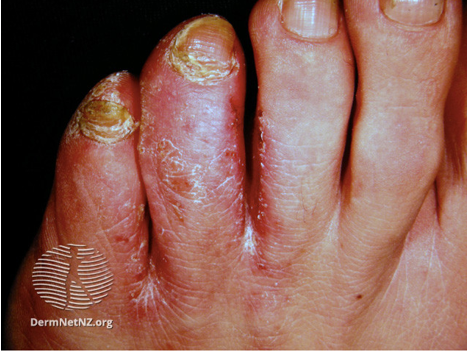
Image 6: Tinea pedis
Image source: Dermnet
|
 |
Treatment
- Dermatophyte skin infections (tinea corporis, tinea cruris, tinea pedis, tinea manum) can often be cured with topical therapy alone
- Systemic therapy is generally reserved for severe or refractory infection, or in immunocompromised patients
| Dermatophyte skin infections (tinea corporis, tinea cruris, tinea pedis, tinea manum) |
| Drug |
Application frequency |
Duration |
Notes |
|
Terbinafine 1% cream
|
Apply to the affected area every 12 hours
|
1-2 weeks
Tinea pedis – 2 weeks
|
Not recommended for children under 12 years as insufficient data on safety
|
|
OR
Clotrimazole 1% cream
|
Apply to the affected area every 8 to 12 hours
|
4-6 weeks
|
First choice for tinea cruris and Candida skin infection.
To prevent relapse, treatment should be continued for at least two weeks after the disappearance of all signs of infection.
|
|
OR
Miconazole 2% cream |
Apply to affected area every 12 hours
|
2 – 6 weeks
|
Continue for 7 – 10 days after lesions have healed.
|
When to take samples
Note: sensitivity is not 100% , approximately 1 in 3 samples will return a false negative result for fungal infection.
Take samples for fungi:
- in severe or extensive skin fungal infections
- skin infections refractory to initial treatment when the diagnosis is uncertain
Skin sampling instruction
- Swabs are of little value for dermatophytes, unless there is insufficient material obtained by scraping
- Wipe off any treatment creams before sampling
- Keep any samples at room temperature. Do not refrigerate as dermatophytes are inhibited at low temperatures, and humidity facilitates the growth of contaminants
- Samples should be collected into folded dark paper squares. Secure dark paper squares with a paper clip and place in a plastic bag, or use commercially available fungal packets
Skin scrapings
- Scrape skin from the advancing edge of lesion; use a blunt scalpel blade or similar
- 5mm2 of skin flakes are needed for microscopy and culture
Reviewed December 2022
